


Nearly all individuals during their teen years are affected to some extent by acne. Acne even affects some people well into adulthood, making it the most common type of skin condition. Acne affects both men and women and most commonly occurs on the face, neck, back, chest and upper arms. Although it is generally not considered a serious health condition, it may cause embarrassment and even scarring of the skin in severe cases. Even if you are affected by severe acne, there is good news! There are a variety of different treatment options available to treat acne that will help restore a smooth, healthy glow to your skin.
Before you learn how best to treat your acne, it is important that you understand the basics of your skin’s anatomy and how acne occurs. Your skin is composed of two layers known as the epidermis and the dermis. The epidermis is the skin’s primary defense against the environment. The dermis is primarily composed of collagen and elastin fibers, which provide the skin with structure, support, and elasticity. Blood vessels and nerves run throughout the dermis. The blood vessels transport blood, which supplies important nutrients to your skin and the nerves allow you to perceive sensations like pain, temperature, and touch. Your skin has many pores, which are actually small openings in the skin from sweat glands, hair follicles, and sebaceous glands deep within the dermis.
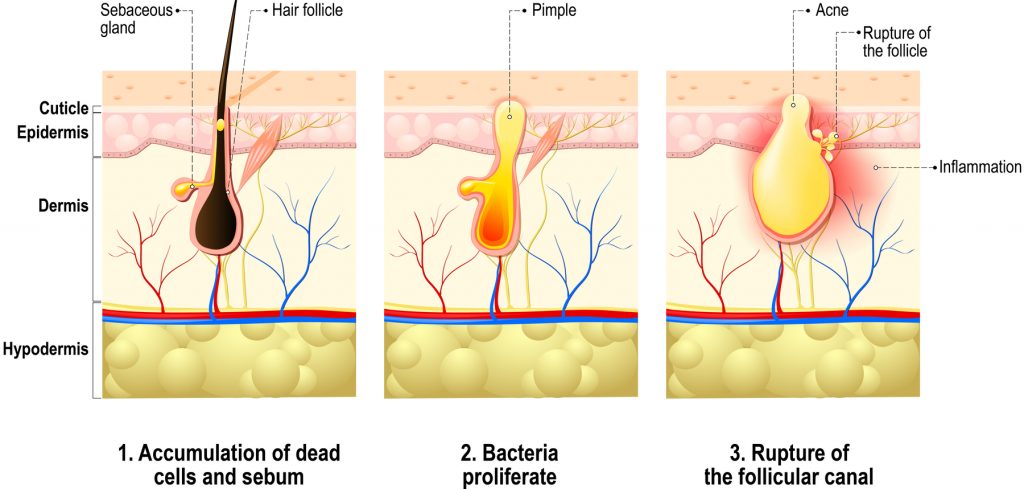
Acne results from clogged pores. What you may not know is acne generally occurs in sebaceous glands that are attached to hair follicles—not sweat glands. The greatest number of sebaceous glands is found on the face, neck, and back, which is why acne commonly occurs in these regions. Sebaceous glands are special glands attached to the hair follicle. Together, the hair follicle and sebaceous gland are often referred to as the pilosebaceous follicle. Sebaceous glands produce an oily substance known as sebum, which helps make your skin waterproof and prevents it from drying out.
You have probably heard that things like chocolate, soda, and greasy foods like pizza can cause acne. While this may be true for very select individuals, physicians do not generally believe this to be the case. Acne is usually caused by a combination of factors including a build up of dead skin cells, excessive sebum production, and bacterial overgrowth. As these factors become more severe, so too does the acne. What starts out as mild acne may progress into moderate or severe acne, depending on the conditions in your skin. Let’s take a look at how these different stages of acne develop.

Dead skin cells are continuously shed from the walls of hair follicles during a process known as keratinization. Under normal circumstances, the skin cells do not build up and the sebum is secreted onto the skin’s surface. However special conditions can promote an increase in keratinization. If too many skin cells build up in the follicle, they may actually block the secretion of sebum, which causes a plug to form. This plug is what is commonly known as a blackhead or a whitehead, which are mild forms of acne. Blackheads generally appear as small, black holes on the skin’s surface. When the follicle is not completely blocked, it opens slightly and the top of the plug turns black, which is what you see as a blackhead. In contrast, whiteheads generally appear as small, skin-colored bumps beneath the skin’s surface. The follicle opening is completely blocked with sebum and dead skin cells, which is what you see as a whitehead.
Acne formation gets even more complex. In response to hormones known as androgens, like progesterone and testosterone, the sebaceous glands produce more sebum. This is why acne usually starts to occur during puberty and why women may experience more acne at the onset of menstruation. When excess sebum is produced in already blocked pores the follicle becomes inflamed. Further inflammation can be caused by bacterial overgrowth as well. Together, this causes a papule to form, which is a red, raised bump on the skin.
Continual sebum production and bacterial overgrowth increase the inflammation around the follicle even further. Like a dam that cannot hold any more water, the follicle may eventually rupture, spilling its contents into the skin layers below. When this happens, pustules form. This is because your body sends white blood cells to the area as an immune response. These white blood cells along with other debris create pus, which is what gives pimples their white or yellowish center.
In cases in which inflammation becomes even more severe, nodules and cysts may develop. Nodules are large, round bumps that originate deep beneath the skin’s surface. They are typically caused by severe inflammation and infection within the dermis. Although similar to nodules, cysts are usually filled with pus. Both of these types of acne may be long lasting and painful. In addition, nodules and cysts may lead to acne scarring and generally only respond to intense forms of treatment.
Antibiotic treatment has been a standard approach in treating acne for many years. Available in both topical and oral formulas, antibiotics such as erythromycin and tetracycline are often used to treat moderate to severe acne. Antibiotic treatment works by reducing acne-causing bacteria, sometimes by as much as ninety percent. However, unlike benzoyl peroxide, antibiotics work to reduce inflammation as well. This is why dermatologists often combine topical antibiotics with benzoyl peroxide for better results. Your dermatologist may start you off with a high dosage and gradually decrease it as your acne improves over the course of several months. It is important to realize that if you use the same antibiotic treatment for a long period of time the bacteria may eventually develop resistance, which means that the treatment will stop working. However, under these circumstances, different antibiotics can usually be used.
Certain oral contraceptives, or “the pill,” have been found to be effective in treating acne in women. As you learned earlier, sebaceous glands produce more sebum in response to androgens, which promotes acne formation. Oral contraceptives work by reducing androgens. As a result, sebum production decreases, which reduces acne. Oral contraceptives can be used over a long period of time to treat your acne, although it may take a few months for you to notice an improvement in your complexion. It is important to realize that if you stop taking the pill, your acne may return. Although there are many different forms of the pill, not all of them can be used to treat acne. You should discuss the different options with your physician to find the treatment that is right for you.
Clascoterone cream has been available in the USA & Canada for over two years and has rapidly become a popular treatment. It is an androgen receptor inhibitor without any systemic absorption and so suitable for men and women. Clascoterone reduces oil (sebum) production and inflammation. It takes time to work – anywhere between 12 to 24 weeks. It is well tolerated and only causes mild skin irritation, redness and dryness.
Retinoids are Vitamin A derivatives and are available in topical and oral formulas. Commonly used to treat mild to moderate acne, topical retinoids work by unclogging your pores and also preventing new whiteheads and blackheads from forming. Like other acne treatments, topical retinoids can increase the effectiveness of benzoyl peroxide and antibiotics when used together. In contrast to topical retinoids, oral retinoids are only appropriate for the most severe cases of nodulocystic acne. They work by reducing sebum production, limiting the build up of dead skin cells, inhibiting the growth of acne-causing bacteria, and even reducing redness and inflammation. While oral retinoids can produce significant results, they also come with serious side effects such as increased cholesterol, compromised digestive and liver function, and even birth defects. Therefore, you should discuss your health history as well as the possible side effects with your dermatologist to determine if the treatment is right for you.
If individual spots last more than 10 days then there is a high risk of that person eventually developing acne scars. Scars may be ice-pick, hypertrophic or atrophic. Certain topical anti-acne products may limit the development of scars. Scars can be improved but not eliminated by a range of dermatological treatments.
Acne can cause marks especially in non-white skin. These can last for many years before fading - but some never fade away. Treatments are available to help remove these marks and prevent them happening.
The light emitted from Ipulse helps to destroy the bacteria which causes acne by exciting the existing oxygen molcules and increasing the molecules power. These super powered molecules break down the bacteria that cause acne and create an atmosphere where it cannot breathe. By boosing the skin’s internal cleansing system in this way, Ipulse dramatically reduces acne and the occurrence and apperance of scarring, resulting in much clearer skin.
IPL is a recognised treatment for mild to moderate acne. It calms overactive grease glands and removes bacterial infection – particularly when used with specialist skin care.
How does IPL work?
A powerful beam of ordinary light is released as a single or series of short pulses. The light destroys bacteria and shrinks grease glands within the skin. Both are necessary to form acne spots.
How is the treatment carried out?
You will be asked to put on some goggles to protect your eyes. A layer of chilled gel is applied to the area to cool the skin during treatment. A pulse of light is delivered into the skin which last for less than a second. A feeling of warmth or skin pricking is felt with each pulse of light. About 50 pulses may be required to treat the whole face.
Am I suitable for treatment?
Dark-skin or sun-tanned skin (including fake tan) cannot be treated. All make-up must be removed. Certain skin or medical conditions, skin treatments and medicines may exclude a person from treatment. The beard area in men may suffer from permanent hair loss.
Is it safe?
The area is usually red immediately after treatment. This settles in a few hours. Blistering may occur if the light pulse is set too strong or if make-up is left on the, or if the skin is too dark or sun-tanned. This may lead to discoloration of the skin.
How long does each treatment last?
A treatment session can last about 15 minutes.
Glycolic acid peels, topical anti-acne prescription medications and photodynamic therapy can be combined with IPL to maximise results.
How many treatments are necessary?
Typically a course of six IPL treatments with each treatment every 2 weeks are needed. Glycolic acid peels can be done in the alternate weeks.
Consultation procedure
There are a variety of skin complaints that look like acne and types of acne that are not suitable for IPL.
A consultation with a consultant dermatologists* is advised to correctly diagnose your problem, estimate the success of IPL for you and discuss a well as offer the full range of alternative medical treatments available.
Aftercare
Sun tanning after IPL treatment will delay further treatment until it has settled and may cause temporary skin darkening.
*Member of the Royal College of Physicians and Member of the British Association of Dermatologist
Dr Anthony Downs, consultant dermatologist has been managing acne with a variety of patients since 2000. Dr Downs can help you diagnose and treat acne with a bespoke treatment designed to your individual needs.
Mr Downs can offer topical and oral treatments for active acne including isotretinoin, management of acne cysts including steroid injections, removal of post-inflammatory dark marks with topical treatments or lasers and the improvement of all types of acne scars with topical treatments, surgery, steroid injections, vascular lasers and fractionating lasers.
Dr Downs has also been involved as a research collaborator in:
Acne national genetics clinical trial 2009-2014
Acne Publications
